Research
Blood Glucose Management for People with Type 1 Diabetes (Ken Li)
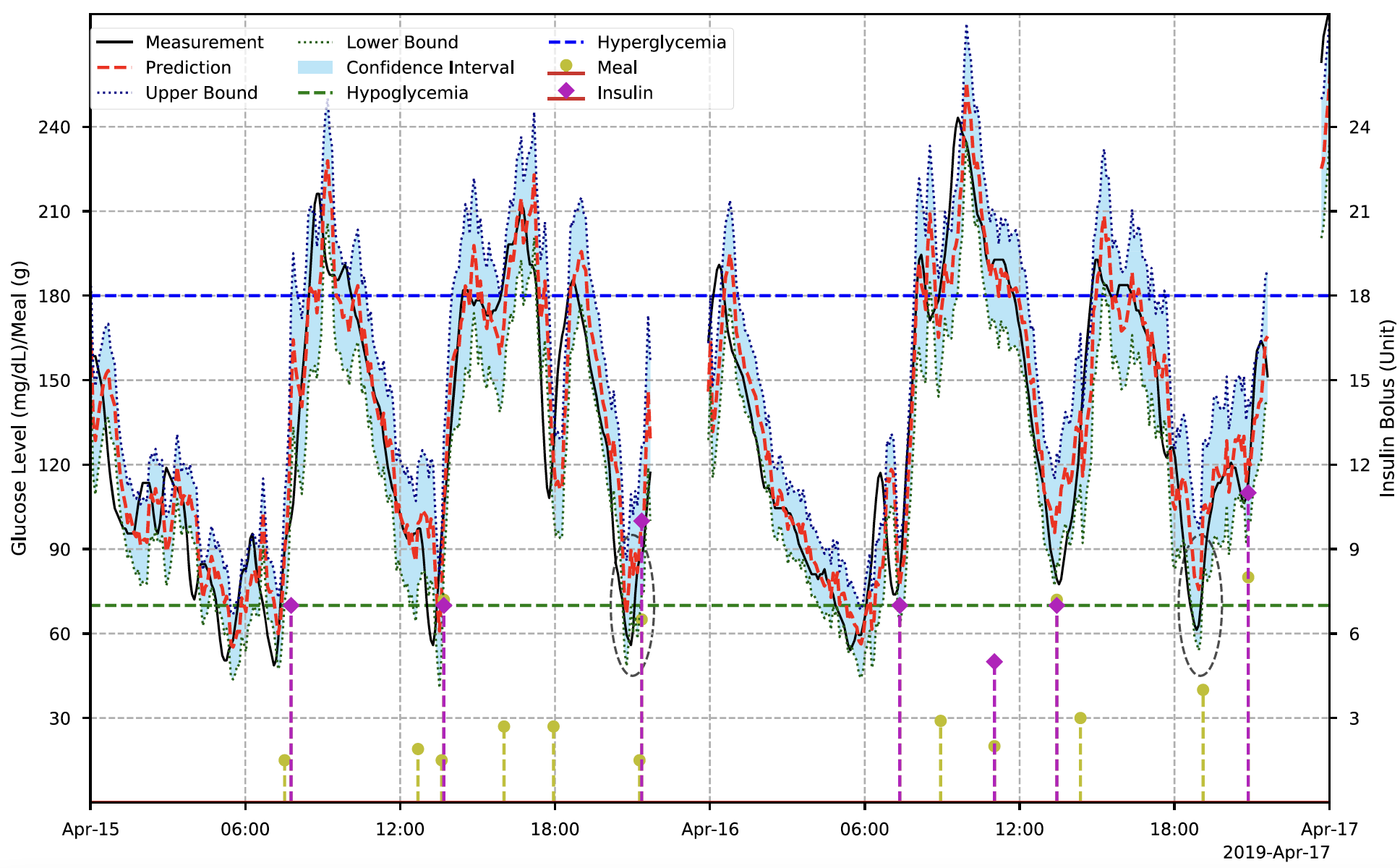
Diabetes is a group of chronic metabolic disorders that affect almost half a billion people worldwide1, and around 10% of them have type 1 diabetes (T1D). Due to an absolute deficiency of endogenous insulin caused by pancreatic β-cell loss, the management of T1D relies on exogenous insulin delivery and adherence to a group of self-care behaviors, such as estimating dietary carbohydrate and exercise, and titrating insulin therapy. The primary objective of T1D self-management is to prevent immediate adverse glycemic events, including hypoglycemia and hyperglycemia, and minimize the risk of long-term diabetes complications. Severe hypoglycemia may cause seizures, brain damage, and intellectual impairment, while hyperglycemia is a risk factor for cardiovascular diseases, neuropathy, nephropathy and retinopathy. The development of continuous glucose monitoring (CGM) has led to therapeutic benefits in diabetes management. The usage of real-time CGM systems has been demonstrated to reduce the number of severe hypoglycemic events for T1D subjects with multiple daily injection (MDI). As a wearable device that automatically measures glucose levels with a fixed frequency (e.g. five minutes), CGM can be combined with an insulin pump as sensor-augmented therapy or an artificial pancreas (AP) for closed-loop glycemic control. MORE INFO
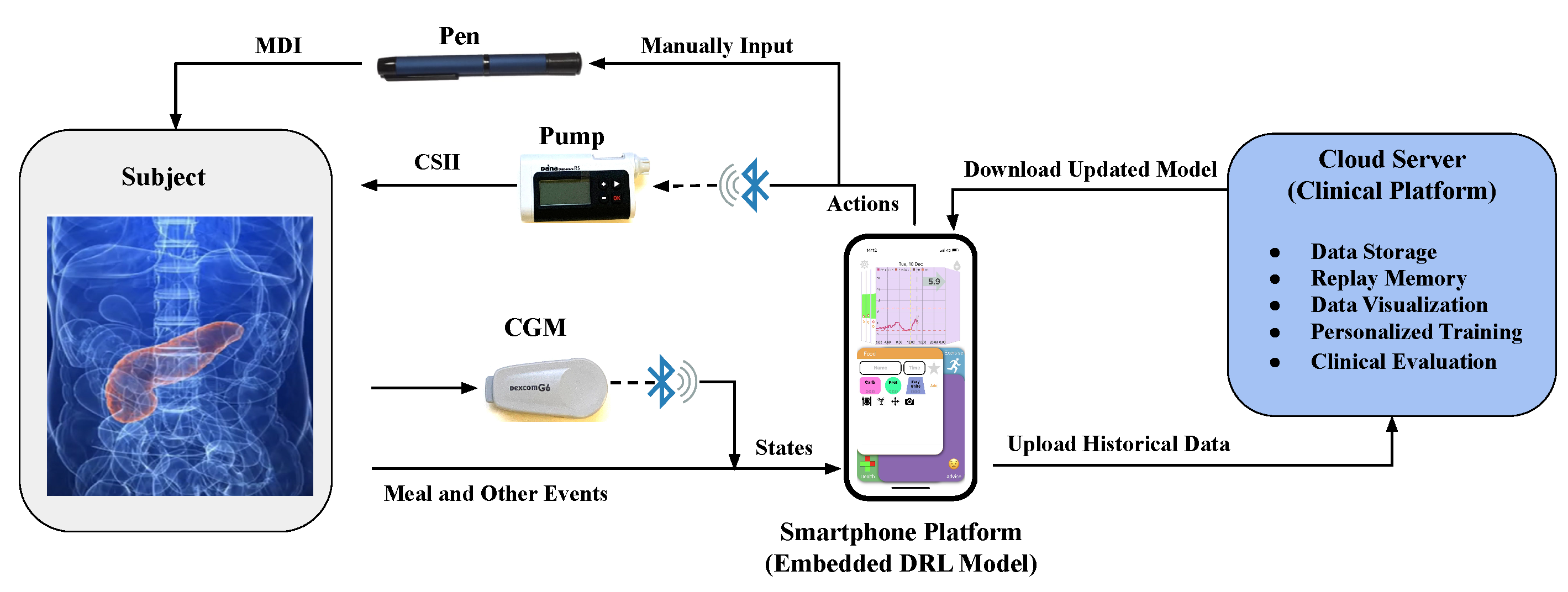
In an AP system, the CGM sensor measures real-time glucose concentration at a fixed frequency (e.g., every 5 min) and transmits the readings to a controller which computes the insulin doses to be delivered by a pump. Reinforcement learning, a sub-field of machine learning, employs a goal-oriented agent to learn the strategies for sequential decision-making, which has been increasingly applied to glycemic control, and in particular, for basal insulin modulation.MORE INFO
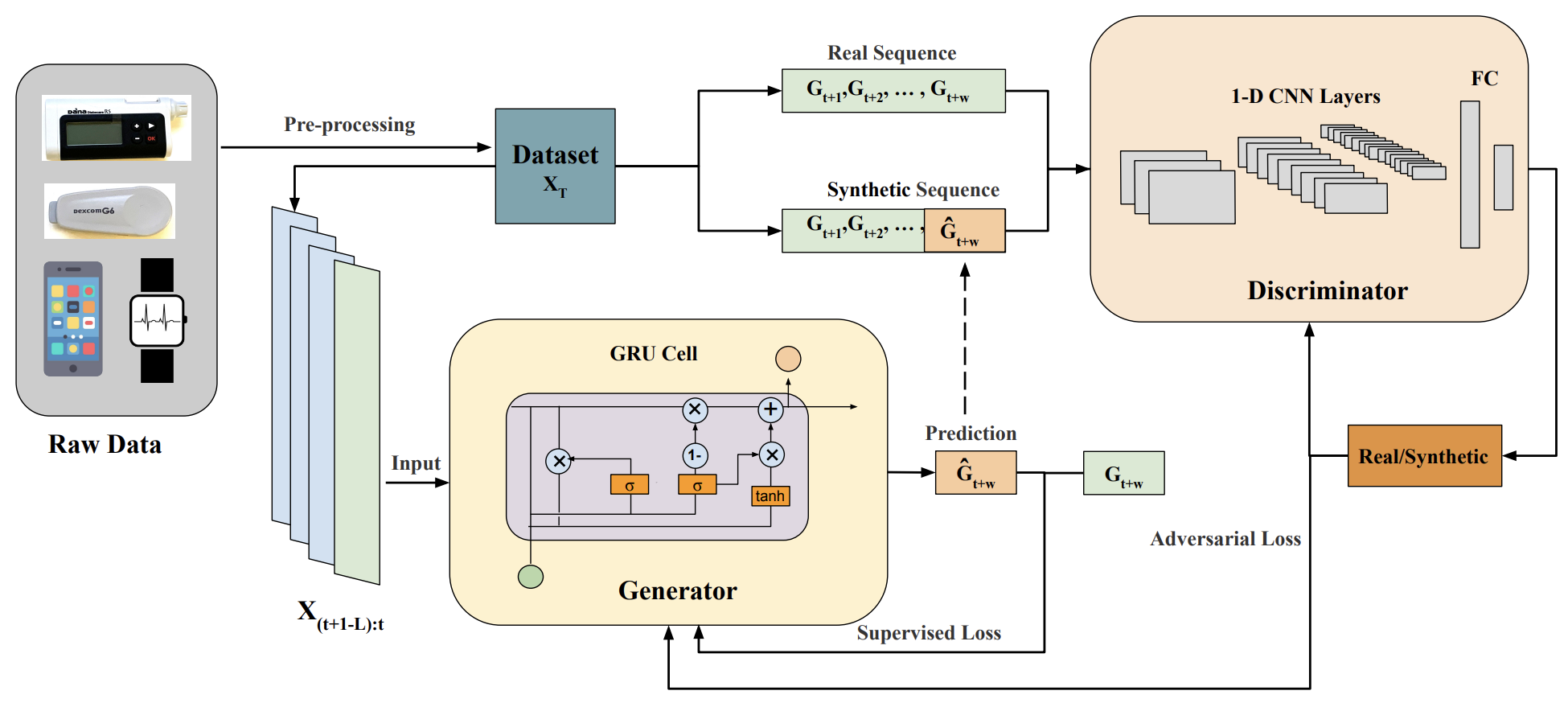
CGM has produced a vast amount of BG data with its increasing use in the diabetes population. Taking advantage of this, the emergence of deep learning algorithms for BG prediction has achieved recent success and outperformed several conventional machine learning approaches in terms of accuracy. Generally, the major challenge of BG prediction lies in accounting for the intra- and interperson variability that leads to various glucose responses under different conditions. Furthermore, many external events and factors can influence glucose dynamics, such as meal ingestion, physical exercise, psychological stress, and illness. Deep learning is powerful at extracting hidden representations from large-scale raw data, making it suitable for accounting for the complexity of glucose dynamics in diabetes.MORE INFO
Improving Healthcare and Outcomes of Critically Ill Children During Transport to a Higher Level of Care (Zhiqiang Huo)
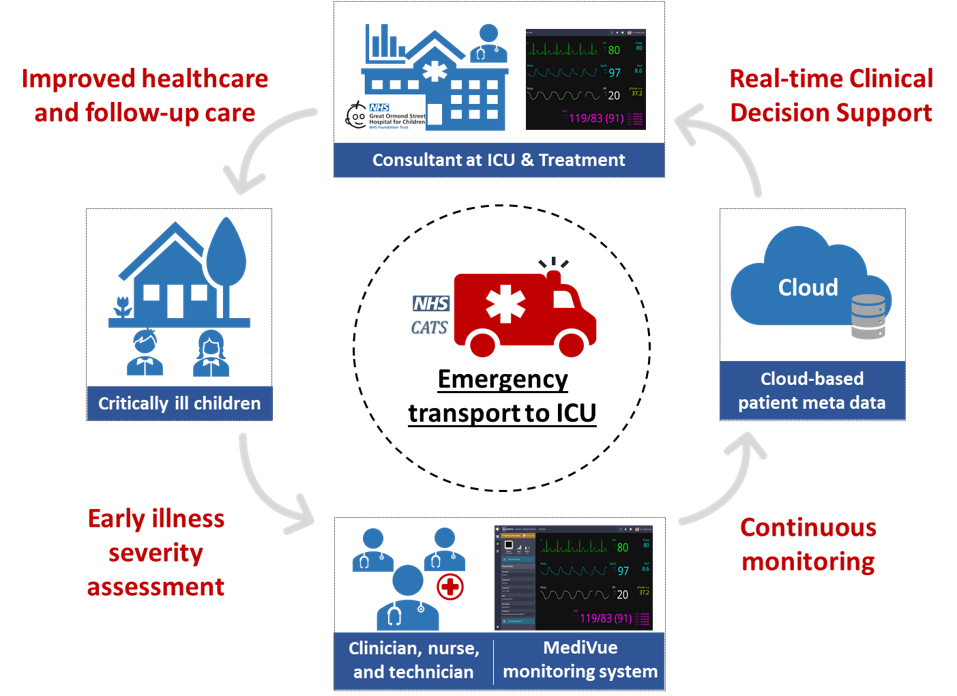
“A healthy person has a thousand wishes, a sick man has but one - Berger R, 1986”
The Paediatric patient is a special cohort of patients with a wide age range from birth through to aged 16. They need careful care and specialized treatment and intervention due to their complexity. Due to developmental disease, some children need to be referred and transported to receive a higher level of care in a children’s hospital. During transport, patients are likely to experience health deterioration and poor outcomes. Our work aims to early detect patients who have a deteriorating health condition in a proactive fashion using continuously monitored patient vital signs and advanced artificial intelligence. More importantly, this will help dedicated intensivists make better decision-making whilst the whole course of transport, medication and intervention to improve the health care and outcomes of patients.
Real-time Aggregated Prediction of Hospital Admission for Emergency (Zella King)
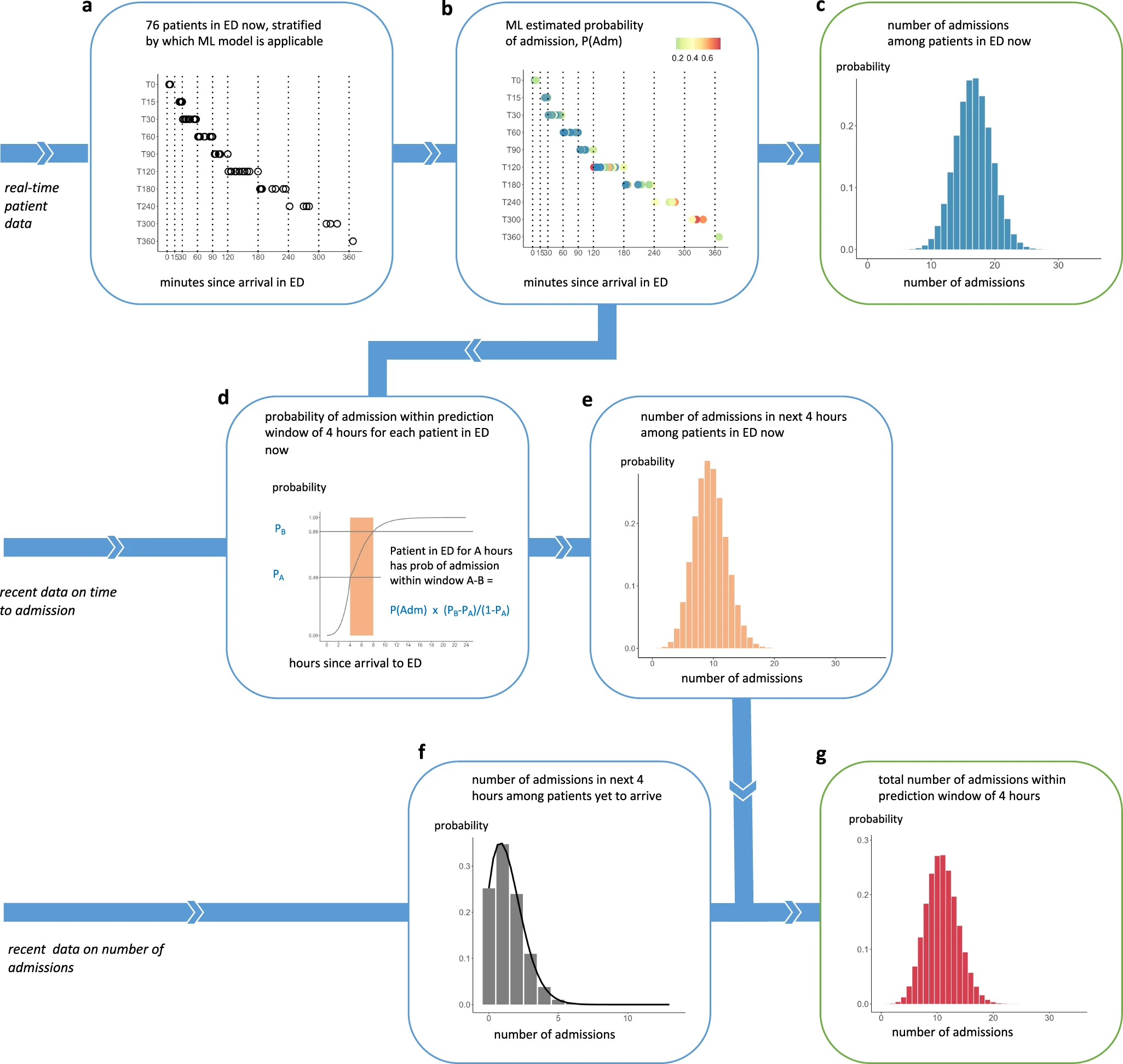
To date, most applications of Artificial Intelligence (AI) to healthcare have been applied to address clinical questions at the level of individual patients. Now that many hospitals have electronic health records (EHRs) and data warehouse capabilities, there is the potential to exploit the promise of AI for operational purposes. Hospitals are highly connected systems in which capacity constraints in one area (for example, lack of ward beds) impede the flow of patients from other locations, such as the emergency department (ED) or those ready for discharge from intensive care. Arrivals to the ED show diurnal and seasonal variations, with predicted peaks in the morning and early evening, but workflows elsewhere in a hospital mean that discharges from the hospital happen late in the day, creating flow problems. This mismatch of cadence between different parts of the hospital results in patients boarding in ED, or being admitted to inappropriate wards, with adverse consequences including longer stays, greater risk of medical errors and worse long-term outcomes in elderly patients.
Hospital services can be managed more efficiently if accurate short-term forecasts for emergency demand are available. Currently, most hospitals use simple heuristics to make short-term forecasts of numbers of emergency admissions, which are based on rolling averages for each day of the week. Maching Learning (ML) is attractive for such predictions because its aggregation of weak predictors may create a strong prediction model. MORE INFO